Equine anthrax is highly fatal, contagious, a bacterial disease of all warm-blooded animals including horses. The horse, like humans and pigs, is less susceptible to equine anthrax than ruminants. Nevertheless, when a horse is infected with Bacillus anthracis, the course of the disease is acute, and death usually occurs within days.
What are the Causes of Equine Anthrax?
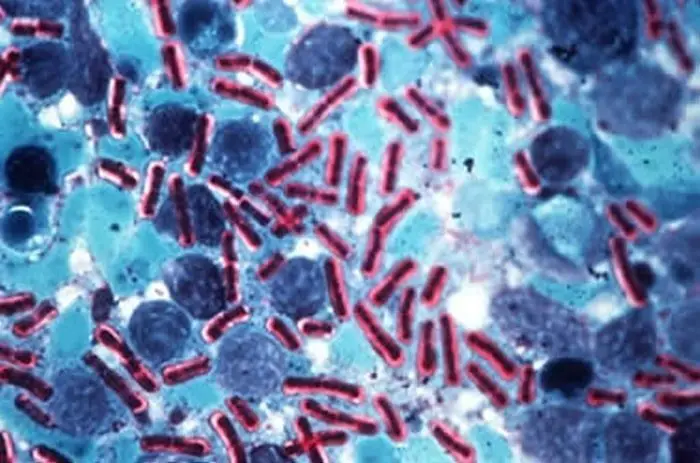
- Bacillus anthracis is a large, non-motile, gram-positive rod( about 4-8 micrometers long by 1 micrometer wide). It is a strict aerobe that grows well between 12° C and freely produces its highly resistant spores between 15° C and 40° C.
- The square-ended vegetative cell is surrounded by a large capsule composed of a polyglutamic acid, which is induced by a plasmid. The capsule is always formed in vivo by virulent strains but only in particular circumstances in vitro.
- Vegetative cells sporulate in the presence of air. The production of spores in the diseased animal is inhibited by buffering and carbon dioxide.
- Unlike the vegetative forms, the spores are resistant to most disinfectants unless they are applied for lengthy periods at comparatively high temperatures.
- Peracetic acid is useful sporicide but the spores are only readily killed by steam under high pressure.
- The organism is readily cultivated in the laboratory and produces a highly distinctive growth. Each large, rough colony is non-hemolytic, looks like a piece of frosted glass and because the bacilli grow in long who is at the periphery, it has been likened to the Medusa’s head.
Epidemiology and Pathogenesis of Anthrax
- The persistence of B anthracis as a threat to animal health depends on a combination of environmental factors.
- There are well-recognized enzootic zones in the world(e.g., parts of the Indian subcontinent, Africa, North, and South America) in which circumstances regularly favor the organism.
- In these areas, the existence of alkaline and calcareous soils with suitable amounts of nitrogen and a combination of a warm temperature (frequently >15° C) with periodic wetness promotes abundant multiplication of the vegetative bacilli.
- Decreases in the humidity and temperature in these enzootic areas promote sporulation, and spores further augment the extensive contamination of the soil and vegetation from the carcasses of animals dying from the disease.
- The anthrax spores can survive in the soil for more than 60 years. Repeated, if unpredictable, epidemics of infection occur in these zones unless control measures are implemented.
- Outside these zones, anthrax is a much more sporadic disease, the occurrence of which depends either on exposure to the accidental introduction of spores on vegetable foodstuffs or animal products or to the disturbance of soil contaminated in the past by buried anthrax carcasses.
- These circumstances prevail in the UK and more generally in western Europe.
- Sometimes in the subtropics, biting flies inoculate b anthracis into the skin, but in general, anthrax is contracted by inhaling the spores.
- When ingested, the spores lodge in the pharyngeal or enteric mucosa, germinate and encapsulate.
- The capsule prevents phagocytosis and destruction of the cell.
- The vegetative cells begin to produce toxins. The complete toxin is a complex of substances, which are encoded by a plasmid.
- One component of the toxin is adenylyl cyclase, which provokes massive edema at the site of invasion.
- The event favors further multiplication and dissemination of vegetative cells into the lymphatic system.
- Bacteraemia and septicemia occur when the lymphatic tissues can no longer contain the agent.
- Death usually follows within a few hours. The circulating toxin is also produced general impairment of phagocytosis, capillary permeability, irreversible damage to the clotting mechanism, and shock with renal failure.
- It is important to appreciate that in acute anthrax, the production of lethal amounts of toxins precedes septicemia by several hours.
Clinical and Pathological Findings of Equine Anthrax
- The onset of disease in the horse is sudden, and the course brief with few prodromal indications.
- Marked subcutaneous swelling develops in the more dependent parts of the neck, thorax, abdomen, and genitalia.
- Fever and extreme depression accompany severe colic and dysentery.
- Death follows these signs in a day or two.
- Rigor mortis is incomplete and unclotted; tarry blood oozes from the orifices of the body.
- The pathological picture is one of hemorrhagic edema and vascular damage throughout the body.
- There are hemorrhagic necrosis and gross swelling of the lymph organs.
How is anthrax diagnosed in Horses?
- In many countries, including the UK, anthrax is a notifiable disease, and even a suspicion of its possible occurrence must be reported to the appropriate authorities.
- Diagnosis in a freshly dead animal is made in the first instance by microscopic examination of blood smears.
- The blood should be collected from a small superficial vein that is likely to ooze little when opened.
- Swabs of this blood are also usually required. Any leakage from the vessel should be staunch with swabs soaked in strong disinfectant, or the vessel should be cauterized.
- Smears should be reasonably thick and lightly fixed before staining with polychromatic methylene blue (or Giemsa).
- The slides should be handled with caution because spores are likely to be present.
- The presence of blue, “square ended” bacilli surrounded by large pink capsules which frequently have frilly edges is conclusive. These bacilli are often in short chains.
- Bacillus anthracis can readily be isolated from the swabs either directly or by sacrificing the skin of a laboratory animal such as the Guineapig with the swab.
Treatment and Control of Equine Anthrax
- Equine anthrax is very sensitive to a wide range of antibiotics, including Penicillin and Tetracyclines.
- These drugs are curative if administered in massive doses to an animal in the early stages of the disease before the toxin has produced irreversible damage.
- They also prevent the development of the disease in other animals within a group deemed to be at risk from exposure to a common source of infection.
- In areas where the disease is known to constitute a more or less continuous threat, annual vaccination of all grazers is necessary.
- The stern vaccine contains viable spores that produce living cells of B anthracis that lack the genes which encode the capsular material.
- They cannot, therefore, encapsulate when they germinate in vivo. Such cells survive only briefly when the spores are inoculated in the animals, but they live long enough to elaborate toxins.
- Both factors II and III are immunogenic and stimulate antibody production.
- Antibody to the receptor binding molecule (Factor-II) prevents factor I and III from acting on cells.

- If there is even the slightest region on clinical grounds to suspect anthrax, high circumcision is required in handling the case to minimize the risk to all the people and any other animals directly or indirectly associated with it.
- The circus should not be the subject of a post-mortem examination for this procedure favors a massive release of spores into the environment.
- Control measures vary in detail from country to country but always include prompt and effective disposal of carcasses, disinfection of building, bedding and equipment, and quarantining of contacts, with additional controls of their produces.