Horse allergy is a severe respiratory problem in the equine family. In this condition, the horse’s saliva and cells can trigger an immune system and as a result, may arise sneezing, different types of an allergic reaction, asthma, and others. There are various categories of horse allergic diseases, and their causal agents, sign, treatment, and prevention are varied. Horse allergy may be simple but will cause serious issues during the performance of your horse.
5 Basic Types of Horse Allergy
There are many types of horse allergy like urticaria, angioedema, inhalant allergic dermatitis, food allergy, allergic contact dermatitis, and culicoides hypersensitivity. I shall discuss five major horse allergy with clinical signs, diagnostic procedures, treatment and control measures for easy understanding for the horse owner.
1.Urticaria and Angioedema
Urticaria and angioedema are usually manifestations of type-1(immediate) hypersensitivity reactions. Antigens which have been implicated include insect bites and stings, feedstuffs and additives, drugs, vaccines, infectious agents, parasites, topical applications, pollens, dusts fungal and spores. The appearance of an urticarial reaction may be triggered by non- immunological factors such as heat, cold, exercise, stress, and physical pressure (dermatographism), but there is usually an underlying hypersensitivity state.
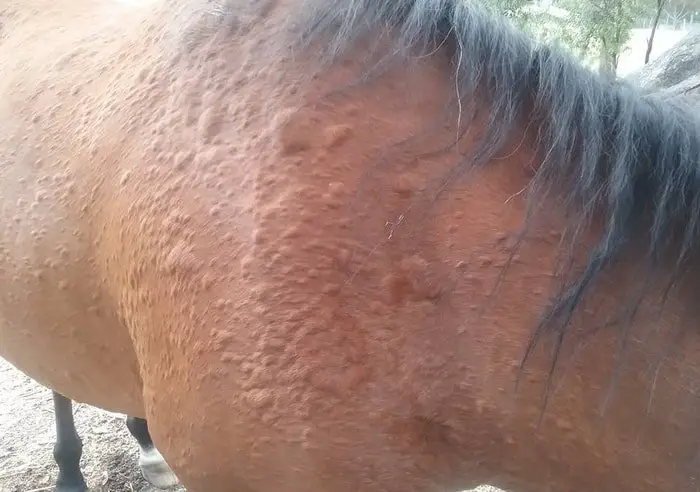
Clinical Signs
Urticaria or hives is characterized by the presence of multiple oedematous swellings in the superficial dermis, often widely distributed over the body surface. The overlying epidermis is healthy, although the accumulation of fluid in the dermis may result in overlying hairs appearing to stand up from the rest of the haircoat. Angio-oedematous plaques are larger in size and arise deeper in the dermis and are more often associated with serosanguinous oozing from dependent skin surfaces and subsequent crusting.there may be associated pruritus, although some animals seem and unaware of the lessons. Urticaria may occur as a single episode only or may be chronic, with repeated episodes experienced over a while.
Diagnosis Procedures
The appearance of the clinical signs is typical. However, the identification of the underlying cause of the hypersensitivity reaction can be complicated. A thorough history of diet, management regime, and recent drug exposure is essential. A restriction or exclusion diet may be indicated. Alterations in management routine and intradermal skin testing may be employed in efforts to identify the causal allergen.
Treatment and Control
In the acute phase, clinical signs can be reversed, often rapidly, by parenteral administration of glucocorticoids. In chronic cases, all attempts should be made to identify and subsequently, avoid the causal allergen. If this is not possible, then oral administration of prednisolone at a dose rate of 0.5-1 mg/kg/day should control the condition.antihistamines may help prevent the appearance of lesions and also reduce the steroid dose requirements. Hydroxyzine hydrochloride at doses of 200-400 mg b.i.d. Has been reported to be effective.
2. Inhalant Allergic Dermatitis/ Atopy
Hypersensitivity reactions may occur to inhaled allergens such as tree, grass and weed pollens, dust, animal, and human danders, fungal, and mold spores. The reactions may be type 1(immediate) and type IV (delayed).
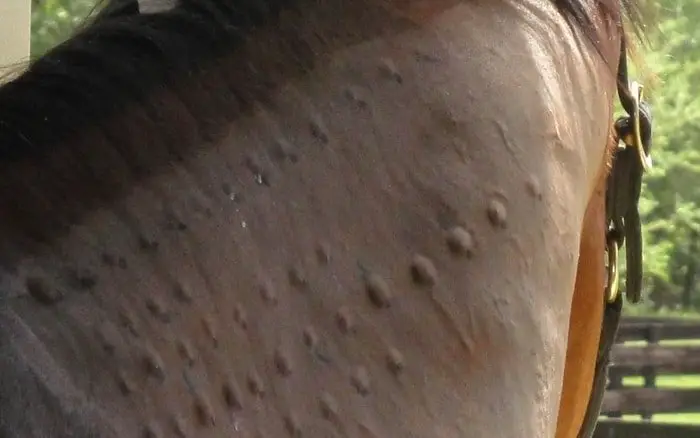
Clinical Signs
Clinical manifestations of hypersensitivity to inhaled allergens may affect the skin and respiratory systems, and allergy has also been implicated in some horses which head-shake. Cutaneous signs include marked pruritus with no primary lesions and chronic urticaria. Secondary injuries due to self-trauma may develop, such as excoriations, hair loss, thickening of the skin, and lichenification. The condition may be seasonal in nature, and the age of onset is usually between 1 and 4 yr. As in other species, a genetic predisposition to develop allergy is likely.
Diagnosis Procedure
Food hypersensitivity and insect or parasitic hypersensitivity reactions must be ruled out. A tentative diagnosis can be made on history, clinical findings, and ruling out other differentials. Circulating eosinophilia may be present. Skin biopsy often reveals tissue eosinophilia, increased numbers of mast cells, and superficials perivascular inflammatory infiltrate. Intradermal skin testing is indicated to confirm the diagnosis and to identify causal allergens. Drugs, stress, and other factors may influence skin test results, and testing is best performed by experienced operatives, using proven allergen kits.
Treatment and Prevention
Avoidance of implicated allergens is the treatment of choice, which may necessitate significant changes in management and feeding regimes. Hypersensitization has been reported to be helpful in some cases. Pharmacological agents may be required to control symptoms and would include antihistamines and glucocorticoids. Hydroxyzine hydrochloride at doses of 200-400 mg b.i.d. Has been used, but other antihistamines may also be helpful. Prednisolone at doses of 0.5-1 mg/kg, initially daily, will control symptoms, but should be administered on an alternate day basis long term. Essential fatty acids supplementation may be helpful in the management of the condition. Owners should be warned about the possible inherited basis of atopy in the case of breeding animal.
3. Food Allergy
Allergic response to ingested allergens may be manifested by changes involving the alimentary tract, respiratory system, and the skin. They are produced following the initiation of type I (anaphylactic) and type III (immune complexes) and type IV (cell-mediated) hypersensitivity responses. Sensitization can occur suddenly for the first time at any age. A severe reaction may be noted following any subsequent challenge by tiny amounts of the relevant allergen.
Clinical Signs
Skin responses which may be associated with ingestion of food allergens in the sensitized horse include generalized pruritis with no evidence of microscopical skin changes, widespread generalized urticaria, edematous plaques with pruritus with or without swelling of the head and vulva, or generalized pruritus accompanied by inflammation leading to generalized seborrhoea. Cutaneous changes will start to become apparent within 12 hrs of ingestion of the relevant allergen and, without further challenge, will persist for at least 3 wk due to the prolonged elimination of food substances from the alimentary tract.
Diagnosis Measures
Diagnosis of food allergy in the horse is protracted as skin tests, and serological tests are unreliable for this purpose. Initially, all suspect cases must be placed on an elimination diet. As food allergy has not recorded in association with hay or grass, cold-blooded animals should either be turned out to pasture or fed only on hay and bedded on hay or savings.
It is essential to be aware that inhalation of allergens during feeding may result in allergic rhinitis, conjunctivitis, asthma, and cutaneous signs in sensitized animals. Food allergens may initiate such reactions, but they are more frequently encountered in association with inhalation of dust, fungal spores, yeasts or mite debris.
4. Allergic Contact Dermatitis
Allergic contact dermatitis results from a type IV (cell-mediated) allergic response to an agent which has been repeatedly directly to the skin.
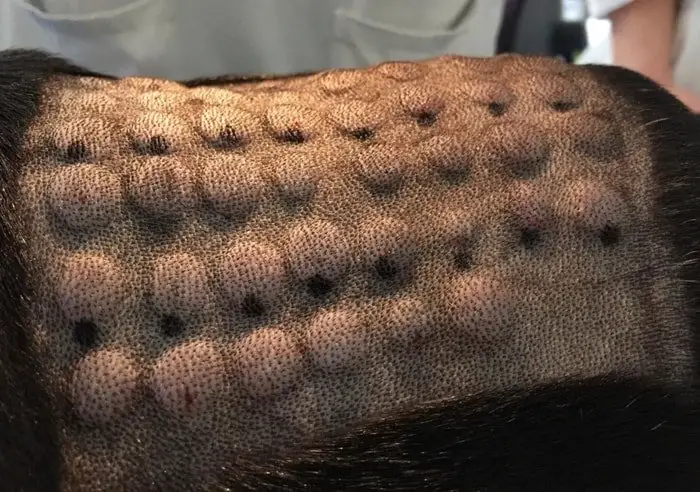
Clinical Signs
The lesions of allergic contact dermatitis are confined to the areas of challenge. They may present as distinct areas of hyperemia, scaling and irritation, cutaneous edema, exudation and irritation with varying degrees of hair loss, or pruritus only. If the condition continues undiagnosed and untreated, secondary changes including skin thickening, increased pigmentation, extensive hair loss, and secondary infection may occur.
Diagnosis Procedures
A close study of the skin change and their distribution will usually indicate as to the possible allergens responsible. Responses to fabrics are uncommon, but allergic reactions to dyes in blankets, rugs, and numnahs will be encountered as will reactions to chronic tanning agents in harness. Less frequently reactions to skin washes and dressings and individual plants may occur.
Horse Allergy: Treatment and Prevention
Having identified the source of the allergy steps should be taken to prevent further contact, like sensitivity, once established, will persist throughout life. Even after further communication has been prevented, irritation is likely to continue for some time, and it is essential that affected areas are gently but thoroughly washed to remove as much allergen as possible. It is necessary in some cases to use short-acting systemic steroid therapy.
Confirmation of the diagnosis may be obtained by patch testing an area of skin either with the agent concerned or an extra and observing the area every 8 hr for at least four days for evidence of local irritation or other skin changes. Independent test sites include the sides of the face and neck. Unless the hair is concise, clipping is advised before application of suspect agents. Skin biopsy of test sites may be undertaken to demonstrate the typical histopathology of allergic contact dermatitis.
5. Horse Allergy: Culicoides Hypersensitivity
Type I and IV hypersensitivity reactions to the bites of Culicoides spp are the cause of the syndrome also known as “sweet itch,” “Kasen,” “Queensland itch,” “muck itch,” “Dhobie itch” or “Sommerekzem.”
In most geographic locations these insects feed primarily at dusk and dawn, less so during the night, and not during the day. Windless conditions with temperature above 10 degrees C are ideal for their activity. Culicoides spp breed in areas of the moist, muddy ground around ponds, marshes, ditches, and tidal flats.

Horse Allergy: Clinical Signs
The onset of these problems occurs between 1 and 4 yr of age or between 1 and 4 yr after the first exposure to the insects. It is seasonal, occurring in the summer and early autumn. In tropical and subtropical locations the season may last for 9 to 10 mo of the year. Pruritis is the ultimate manifestation of this condition and causes self-inflicted lesions. The classically described disease affects the head, ears, mane, withers, rump, and tail. The pruritis experienced by hypersensitive horses causes rubbing and which results in alopecia, lichenification, crusting, erosions, ulcerations, fissures, wrinkling or corrugation of the skin, and secondary infections.
Diagnosis Measures
Diagnosis should be done based on history, and clinical signs, intradermal skin testing, unavailable expect at research facilities, is a useful method for confirming the clinical diagnosis. Biopsy findings of perivascular cuffs of mononuclear cells and eosinophils suggest allergic dermatitis but are not diagnostic for an aetiological agent. The parasitic manages, other insect hypersensitivities, and cutaneous onchocerciasis should be ruled out.
Treatment and Prevention
Treatment requires the prevention of further exposure to the insects and relief of inflammation. Exposure to the insects is eliminated by housing in insect-proof stables from late afternoon until well after dawn. Daily to the twice-daily application of insect repellents contaminating permethrins may be useful, but is likely to be ineffective without stabling. Fine-mesh screening or netting, ceiling fans or strategically placed box fans, and automated insecticide misters may aid in situations where the stables cannot be fully enclosed. Drainage of ponds, marshes and boggy areas where the Culicoides insects breed may be helpful when environmental regulations allow such alterations. Transfer of affected animals to higher, drier pastures or drier geographic locations often results in complete or near-complete resolution of signs.
Inflammation is treated systemically with glucocorticoids. Initial doses of prednisolone or prednisone required to control the severe itch may be as high a 2 mg/kg daily. If insect exposure is not controlled, it is impossible to reduce this dose to lower and safer levels. Some relief of pruritus can be achieved by bathing in tar and shampoos. Secondary bacterial infections should be treated appropriately.
Nightly stabling of affected animals should begin from before the onset of the insect season and continue until the insects subside in the fall. A single night’s exposure during the insect season can cause itching which may last as long as 2-4 wk.
This condition has been seen in related animals, suggesting a genetic predisposition. Affected animals should be removed from breeding programs.
Conclusion About Horse Allergy
If you want to keep your horse in healthy and allergic disease-free condition, then you must have to changes the bedding clothes and grooming your horse regularly. Keep your horse a healthy environment, and the affected animal must have to isolate in the non-affected animal. When your horse affected the allergic disease, it is vital to call a veterinary doctor immediately.