Equine Metabolic Syndrome is a group of conditions in horses that mainly occurs due to imbalance of nutrition intake and absorption. A proper assessment of the dietary nutrition status of healthy working or breeding horses is always a complicated matter, but this is far more complex when there is a superimposed medical problem. The relationship of the nutrition with the development and skeletal growth of horses and foals and a series of Equine Metabolic Syndrome that commonly affect horses are described below.
1. Disturbances of Growth and Skeletal Development
The necessity for correct dietary nutrition of foals, yearlings, and weanlings, cannot be overemphasized, both in terms of work and lifespan of competitive horses. Despite this requirement, few specific details of nutritional necessities are available, and optimal growth rates of tender horses have not been precisely established. This may be why problems of excessive nutrition in young animals appear to be much more prevalent than those associated with undernutrition, as owners assume that the requirements quoted by the National Research Council (NRC) are a minimum.

The significant disturbances of skeletal growth and development in the horses have often been attributed to excesses or of specific dietary components. The umbrella term, developmental orthopedic disease (DOD), is used to describe various disorders of growth in the equine skeleton. These include osteochondrosis, dyschondroplasia, physitis (epiphyseal dysplasia), angular and flexural limb deformities, and cervical vertebral abnormalities ( wobbler disease).
The precise cause of these conditions is unknown, although the primary lesion of osteochondrosis has been defined as a focal failure of endochondral ossification which can occur in both the metaphyseal growth plate and the articular/epiphyseal cartilage complex. It is believed that there is a multifactorial etiology for DOD involving nutrition, heredity, rapid growth rate, endocrinological dysfunction, and biomechanical trauma.
2. Equine Metabolic Syndrome: Overfeeding of Foals
Overnutrition is a cause of osteochondrosis in the horse that has been postulated by many workers, and few lesions of osteochondrosis occur on diets based on the nutritional requirements of the NRC for weanlings growing between moderate (0.65 kg/day) and rapid (0.85 kg/day) rates. Despite proposals that excessive levels of carbohydrate and oil (128% NRC requirements for digestible energy) fed to foals can cause lesions of osteochondrosis. This means that excessive feeding of young horses for weanling and yearling sales is probably detrimental to skeletal development and may lead to clinical problems of DOD when they enter training.

High energy diets appear to predispose to osteochondrosis, irrespective of the average daily gains achieved. High or compensatory average daily gains were thought initially to predispose to lesions of osteochondrosis by increasing the stresses on growth cartilage. Whereas this may be important in some cases, it is likely that growth factors associated with the intake of high energy diets cause abnormal development in the growth cartilage and thus osteochondrosis.
3. Metabolic Syndrome in Horses: Mineral Imbalances
Imbalance of mineral homeostasis is another essential facet of the pathogenesis of osteochondrosis. Foals.foals fed excessive amounts of (e.g., four times NRC recommendation) will consistently show lesions of osteochondrosis, although there may be no clinical signs of secondary nutritional hyperparathyroidism provided adequate calcium levels are fed.
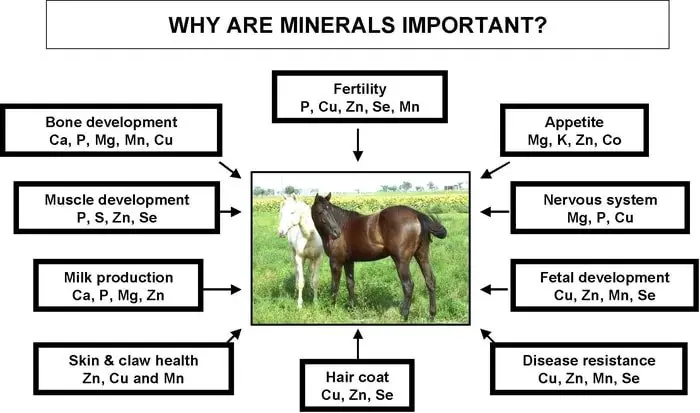
Excessive dietary calcium has also been proposed as a cause of hyper calcitonin ism leading to osteochondrosis and osteosclerosis. There is no evidence to support this theory in foals, but it has been confirmed in fetal lambs whose dams were fed excessive calcium. The levels of calcium recommended by NRS appear to be adequate, and supplementation does not appear to be harmful to the skeletal development of foals. However, increasing the calcium: calorie ratio to foals fed excessive energy (e.g., 128% DE and 340% calcium of NRC recommendations) does not appear to be protective. Lesions of osteochondrosis still develop, which is presumably a manifestation of the excessive energy level.

Copper deficiency in young horses has also been suggested as a cause of DOD. Levels approximating the value recommended by NRC (i.e., 10 mg/kg) have not been associated with an increased incidence of osteochondrosis in foals, as long as the energy and phosphorus components also approximated the level recommended by the NRC. However, it has been reported that copper levels up to 25-30 ppm may decrease the incidence of DOD, especially physitis. The horse has a high resistance to chronic copper toxicity and can withstand levels of ≤800 mg/kg, and so it seems very unlikely that levels of 25-30 mg/kg copper in the feed will have any deleterious effects. The mare can also be fed a higher copper diet during gestation. However, the copper level of mare’s milk is low, irrespective of the dietary copper status of the mare.
No evidence exists that molybdenum restricts with copper metabolism in the horse, as persistent, protein-bound thiomolybdates that occur in ruminants have been unidentified. It is unlikely that diets with excessive molybdenum could cause a copper deficiency and therefore, DOD in horses.
4. Metabolic Syndrome in Horses: Laminitis
Laminitis is the local manifestation of a severe metabolic disturbance. The primary lesion of laminitis is associated with the opening of arteriovenous anastomoses resulting in inadequate perfusion of the dermal laminae. Blood is shunted away from the laminae despite increased blood flow to the foot. Laminitis may occur for a variety of different reasons including fat ponies fed lush pasture, carbohydrate overload (e.g., grain overload), endotoxemia, mechanical overload, post-exhaustion myopathy/laminitis syndrome, the stress of exercise on overweight animals, administration of corticosteroids and constant tube feeding with a high energy/protein ratio.

5. Nutritional Management of Foals with DOD
Foals identified with lesions of DOD must be carefully managed to prevent any exacerbation of lesions and to allow healing to be promoted. Three factors affecting foals with DOD have been identified.
A. Dietary digestible energy level Although little experimental data exist, it appears to be beneficial to decrease the Dietary Energy level to approximately 85% of that recommended by NRC, with100% levels of CP, phosphorus, calcium, and other nutrients. High levels of calcium in combination with high levels of Dietary Energy have not been effective in protecting foals from osteochondrosis, and it is unlikely that excessive levels of calcium assist in the healing of DOD.

B. Dietary copper level: The collagen cross-linking may be enhanced when dietary DM contains higher levels of copper (e.g., 30-45 mg/kg). However, collagen cross-linking is probably sufficient at lower levels (e.g., 10 mg/kg). In cases of physitis, it appears that levels of approximately 30 ppm copper in the dietary DM are beneficial. Since horses have a high threshold level for copper toxicity, the level can be increased with impunity.

C. Exercise and Feeding: The incidence of osteochondrosis increases in foals consuming basal energy diets if exercised. This may be a manifestation of the progression of small, clinically silent lesions into more extensive articular damage due to secondary trauma. If foals are diagnosed with osteochondrosis and/or physitis, then the level of DE fed should be reduced, and any joint trauma decreased by confining the foal and permitting only hand-walking exercise. However, the lack of exercise will further reduce the foal’s DE requirement and 70-75% NRC DE may then be adequate.

6. Equine Rhabdomyolysis Syndrome
Although many predisposing factors have been postulated for the equine rhabdomyolysis syndrome (ERS), diet, fitness, and training regimen remain critical in most cases. Originally fast-twitch (i.e., high glycolytic capacity) muscle fiber degeneration was thought to occur because of muscle glycogen accumulation during a rest period in horses maintained on full rations (i.e., the high level of grain). The glycogen was then assumed to be catabolized with subsequent accumulation of lactic acid. More recently this theory has become less popular with the finding that few horses with ERS have elevated muscle lactate levels or metabolic acidosis and, in fact, any alteration to the status of acid-base balance usually involves a mild metabolic alkalosis.

In general, the acid-base status of horse suffering ERS tends to reflect their fitness and the nature of any other exercise. If the horse is also dehydrated, hypochloraemic or hypocalcemic, then it may be predisposed to a more sustained metabolic alkalosis. Solutions containing bicarbonate should therefore only be given to horses suffering ERS, if necessary, once electrolyte and acid-base status have been determined. However, even in the absence of laboratory facilities for the assessment of electrolyte and acid-base status, isotonic solutions (e.g., Ringer’s solution) should be used to re-establish hydration and induce diuresis (i.e., to diminish the nephrotoxic effects of myoglobin).
7. Equine Metabolic Syndrome: Hyperlipaemia
Hyperlipidemia and hyperlipaemia are the terms used respectively for the subclinical and clinical disorders associated with an elevation in blood triglycerides and lipids. Hyperlipaemia describes the clinical syndrome characterized by anorexia, depression, and hepatic failure and is associated with dramatic increased in blood lipid and fatty infiltration of the liver and other parenchymatous organs. These syndromes are generally precipitated by some form of stress (i.e., transport, alteration of diet, pregnancy, lactation, change of paddock/stabling and infection). Most hyperlipidaemic episodes are associated with reduced dietary intake and in large horses an azotaemic state which exacerbates the condition by restricting the peripheral removal of lipoproteins. During fasting, the triglycerides of fat tissue are broken down into very-low-density free fatty acids and glycerol, which are then came into the blood. In horses, fatty acids taken up by the liver are oxidized fully to give energy or are re-esterified to form triglycerides and phospholipids. These either stayed in the liver or are released into the plasma as very-low-density lipoproteins (VLDLs). In horses, ketone formation is limited; therefore, lipaemia occurs in response to aphagia rather than ruminal ketosis.

Fat, unconditioned ponies are more susceptible to hyperlipaemia than large horses because of the congenital insensitivity of ponies to insulin. The initial treatment regimen involves decreased in the negative energy balance by improving feed intake. If the animal does not voluntarily increase its intake of palatable feed and pasture, then tube feeding of the slurry of readily utilizable carbohydrate or a slurry of a complete pellet must be implemented.
A protocol used for insulin/glucose therapy is 0.15 IU/kg insulin IM b.i.d on days 1,3 and 5 along with 100 g glucose PO b.i.d and 0.075 IU/kg insulin IM b.i.d on days 2 and 4 along with 100 g glucose PO s.i.d. Heparin therapy can be instituted at 40-150 IU/kg b.i.d.although clotting parameters should be monitored with this regimen, especially at the higher levels. If the animal is in fever or in pain, antipyretics and analgesics should be used. The hydration status should also be carefully observed to avoid prerenal azotemia, which greatly exacerbates the hyperlipidaemic condition.
8. Metabolic Syndrome in Horses: Liver Dysfunction
Diffuse hepatic disease interferes with the synthesis of amino acids, plasma proteins, and some clotting factors. It causes decreased glycogen storage, affects formation and excretion of bile salts, excretion of bile pigments and the detoxification and excretion of toxic substances, including photodynamic agents (e.g., phylloerythrin). The hepatic disease often appears clinically as an acute dysfunction, although, as damage to at least 60% of the liver is necessary before clinical signs can be appreciated, the disease is often due to a chronic condition.

Hepatic dysfunction may occur for a wide variety of reasons including viral, bacterial and parasitic infection, hyperlipaemia, biliary lithiasis, neoplasia, and chemical hepatitis. Chronic liver failure may occur after ingestion of plants containing pyrrolizidine alkaloids (e.g., Senecio spp, Amsinckia spp, crotalaria spp, Heliotropium europaeum, and Echium plantagineum). These plants often contaminate alfalfa crops and are incorporated into fodders.
Photosensitization can occur due to slow excretion of photodynamic substances in the bile (e.g., phylloerythrin). This is a natural end product of chlorophyll metabolism, but if biliary secretion is obstructed, then an accumulation occurs. Once a vulnerable concentration is reached at the skin level, then unpigmented, exposed skin is much more sensitive to UV light. Dermal lesions occur on unpigmented skin if the skin is not covered by thick hair or by rugging.

Although hepatogenous photosensitization is most commonly seen when horses are grazing the green pasture, it still may occur on diets of hay and concentrate, as these appear to have sufficient chlorophyll to precipitate the condition. A laxative may be given to removing toxic ingestion but may be of limited value as the hepatotoxic plants may have been ingested up to 6 mo prior to the acute photosensitive condition.

If the dermatitis is severe and antimicrobial therapy is considered, it should be remembered that neomycin causes sequestration of bile salts, which may exacerbate phylloerythrin accumulation. The most useful form of treatment for liver damage involves excellent support and feeding. This involves the provision of IV or oral glucose to fight hypoglycemia. In acute hepatitis, fluid therapy may also be given. The value of protein-rich food to control the crude production of plasma proteins is controversial. However, amino acids, especially mixtures containing methionine, leucine, and valine, are used apparently with excellent results. B group vitamins are also commonly used.
9. Equine Metabolic Syndrome: Wasting Condition
A. Protein-losing Syndromes:
Loss of bodily condition without or with depression of feeding is common in horses and results from many different causes. A significant amount of plasma proteins may be lost in urine (i.e., protein-losing nephropathy), pleural/peritoneal liquids and perhaps most commonly from the gastrointestinal tract. Diets should contain high amounts of quality protein to help in replacement, although in cases of protein-losing nephropathy, it is usually best not to increase protein concentration in the diet as it can exacerbate the azotaemic condition.
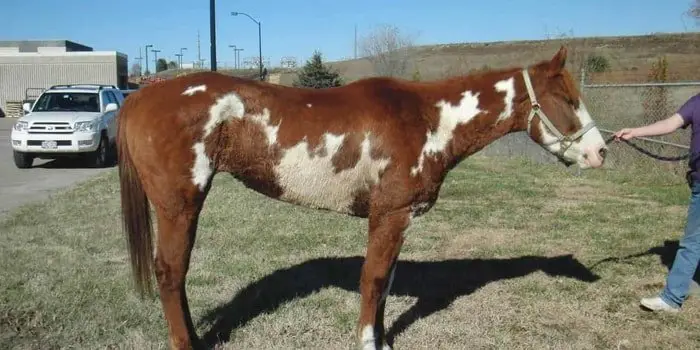
B. Protein-losing Gastroenteropathy
Protein can be removed from the gastrointestinal tract through the loss of mucosal integrity, or lymphangiectasia associated with increased lymphatic pressure. Diagnosis is made by the assessment of the depressed total plasma protein and albumin. In PLGE, the albumin to globulin ratio is constant in the acute stages but decreases if PLGE conditions for more than 4 wks, because the rate of globulin synthesis is much faster than that of hepatic albumin. Albumin has a half-life of approximately 19-21 days. The typical clinical-pathological picture can be obscured if a chronic infection is present and hyper-α and γ-globulinaemia are present, thus increasing the TPP. These mechanisms can be distinguished serum electrophoresis easily.

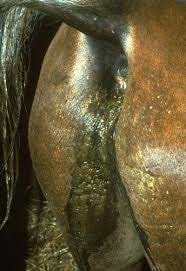
C. Diarrhea or Malabsorption Syndrome
Diarrhea results from the multitude of different causes, including the so-called malabsorption syndrome. The horses with chronic diarrhea often have PLGE as well, usually because of reduced mucosal integrity. They, therefore, require more protein. Normally, they are also in a state of mineral, energy, and vitamin malnutrition. They should be fed ad-lib alfalfa hay, as well as high protein-energy concentrate, a mineral supplement providing calcium, magnesium, zinc, copper and iron and fat and water-soluble vitamins. Horses with chronic salmonellosis usually have impaired fiber digestion, and a diet with an increased proportion of grain/concentrate will help maintain body weight. In some complex cases of chronic diarrhea, the best solution is to turn the horses out into pasture which may promote normalization of gastrointestinal flora.

10. Metabolic Syndrome in Horses: Hepatoencephalopathy
Hepatoencephalopathy is an equine metabolic syndrome, is the result of severe liver disease with impairment of protein, fat and carbohydrate metabolism and detoxification of wastes. The result is hyper ammonia, hypoglycemia, excess short-chain fatty acids, and a relative decrease in the branched-chain aromatic acids, along with the induction of false neurotransmitters in the brain. All play a role in the development of the CNS signs associated with hepatic disease.
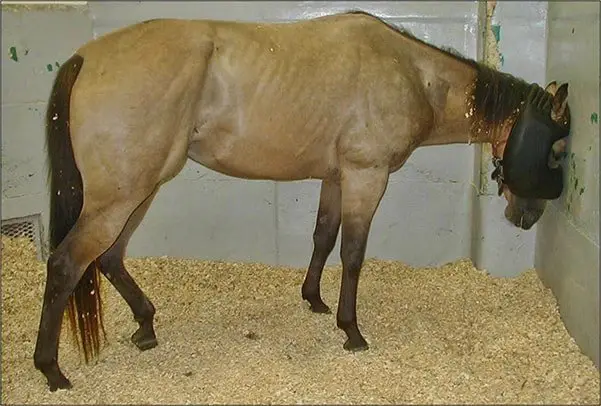
In adult horses, hepatoencephalopathy has been reported in associated with hepatic necrosis due to administration of the tetanus antitoxin, or with liver disease due to the ingestion of the hepatotoxic pyrrolizidine alkaloid-containing plants ( Senecio spp, Crotalaria spp).
11. Equine Metabolic Syndrome: Hypocalcemic and Hypomagnesaemic Tetany
Whilst these conditions are not as common in the equine species as they are in ruminants, they have been reported. In horses, tetany due to low ionized calcium has been occasionally described in heavily lactating, recently transported mares. It is characterized by muscle tremor, weakness, ileus, staggering high-stepping gait, seizures, and “thumps.” Tetany, seizures, and death have been described in critically ill foals with profound hypomagnesemia.

These conditions can be corrected by IV administration of Ca or Mg salt solutions, given of effect, with continual monitoring of cardiac function during therapy. Some animals may require several days of Ca supplementation in order to replace total body calcium deficits.
12. Metabolic Syndrome in Horses: Cushing’s Disease
Cushing’s disease in horses is the result of abnormal activities of the pituitary gland and uncontrolled production of Adrenocorticotropic hormones(ACTH). Cushing’s disease is mainly seen in older horses after crossing the age of 18 to 23. The disease is known by abnormal growth of body hair, weakness, imbalance, abnormal deposition fats in various parts of the body like the base of the tail, neck, crest, and around the heads.

Concluding Remarks of Equine Metabolic Syndrome
The knowledge of Equine Metabolic Syndrome is very important for the horse owner and veterinarian. The syndrome that has discussed in the earlier paragraph is mainly on preliminary ideas, and you need to detail study on each syndrome. I think this article will help you to know about the conditions and you can take adequate precautions much earlier.